
“I feel like it’s my calling to be there,” These are the words shared from Marissa, an ICU nurse in Phoenix, Arizona about volunteering to work in her hospital’s COVID-19 unit.
So why volunteer to put herself at risk every day? After a traumatic hiking accident in 2016 that left her temporarily wheelchair-bound, she says she has a new perspective. “After falling off a cliff and surviving, I have a different attitude. That wasn’t my time to die. If this is my time now, I can accept it.”
She adds that many of her colleagues care for elderly parents or have children at home, so she understands that they may be fearful about putting themselves and family members at risk. “I don’t have kids, so I feel this is something I can do.”
She realizes the personal risk she is taking, even as a younger, healthy person. “I think I have a strong immune system, but then I also realize that may not protect me. This virus brings some people into the ICU with no previous health issues at all. I personally am not seeing as much correlation with pre-existing conditions as you do with other illnesses.”
Change is constant
Marissa, who normally works in the cardiac intensive care unit (ICU), is proud of how well her hospital organized its facility and quickly set up separate areas in the hospital to treat COVID-19 patients. “We have two towers in the hospital so they are able to separate patients and staff,” she says.
Her passion for learning and constant adaptability to change keep her going and focused in this fight. “We are constantly seeing changes in treatment and understanding different symptoms,” she says. “You should be fully able and willing – and that’s how I am. I want to be there.”
The toll on healthcare worker
 Marissa’s feelings and attitudes change from day to day. “I do see hope, but my view changes,” she says. Even when she’s not at work, there are constant reminders of the crisis whether she’s shopping at the grocery store or watching TV. “I had to come to an agreement with my husband that we won’t turn on the television when I’m home. Even if we don’t watch news, all the commercials still reference the pandemic.”
Marissa’s feelings and attitudes change from day to day. “I do see hope, but my view changes,” she says. Even when she’s not at work, there are constant reminders of the crisis whether she’s shopping at the grocery store or watching TV. “I had to come to an agreement with my husband that we won’t turn on the television when I’m home. Even if we don’t watch news, all the commercials still reference the pandemic.”
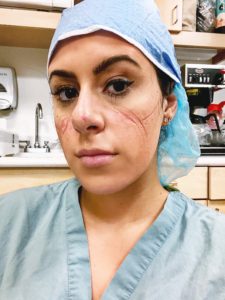
Extended use of PPE also has presented challenges for her and other healthcare workers’ skin. “It puts pressure on the same places on your face over and over,” Marissa says. “I have started taking pain medication because of the swelling. Some nurses have talked about using foam pads, but the hospital told us that may impact the seal of the respirator, which we cannot risk.”
She says her hospital has started reusing N95 respirators and storing them in paper bags. They are supposed to use the respirators until they are unusable. “I know the material is being affected,” she says. “We are sweating and breathing into it for 12 hours.”
Marissa adds they also aren’t allowed to wear make-up or skin care products because it may impact the life of the respirator. “It’s just one more thing that has been taken away.”
Focusing on the bright spots
Marissa says it is heartbreaking to see patients separated from their families and not having the chance to say good-bye to them. “I have to brainwash myself sometimes. I tell myself I’m strong,” she says. But early in the outbreak, she came home one day and her husband had made her a nice dinner and poured her a glass of wine. “I’m not a crier,” she says, “But I just broke down and sobbed.”
“I’m lucky because I have people I can talk to,” she says. It’s easiest for her to talk to coworkers and other friends in healthcare. “And I come from a family of healthcare workers – my parents and my sister – so I can talk to them.” She says talking helps her more than anything, so whether it’s her husband, family, or friends, she is grateful for those around her who help her get through the stress and pain.
She’s also touched by how the families of patients are very appreciative of the nurses. When she worked in the ICU in the past, she said it was not typical for a family to thank her. “Now, people thank us and have even catered lunch for the nurses,” she says. “It doesn’t take much and even the smallest kind gesture can make a world of difference.”
Want to learn more about Marissa’s personal journey both in and outside of healthcare? Follow her on her blog, Sassy Anesthesia or on Instagram.
We want to hear your story from the frontlines of the COVID-19 battle. Reach out to us here.
