On a recent hospital visit, a surgeon told me he’d rather operate on a young, healthy farmer who still has dirt under his fingernails than someone who’s pristinely clean and has been sitting on the couch day after day eating junk food. That viewpoint highlights an important factor in the fight against surgical site infections (SSIs) – you can’t control all the risk factors, so you have to focus on what you can influence.
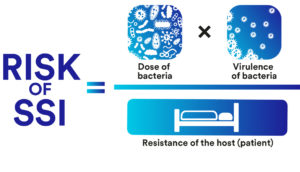
Three variables impact the risk of SSI, according to the Centers for Disease Control and Prevention (CDC): how much bacteria is present, the virulence of the bacteria and the resistance of the host.
 No silver bullet exists to decrease SSIs. It involves monitoring and following procedures throughout the whole surgical process from pre-op to surgery to post-op. It includes the patient, the surgical team, operating room managers, central sterilization and infection preventionists.
No silver bullet exists to decrease SSIs. It involves monitoring and following procedures throughout the whole surgical process from pre-op to surgery to post-op. It includes the patient, the surgical team, operating room managers, central sterilization and infection preventionists.
Although you can’t control the virulence of any bacteria present, as a care provider, you can influence the other two risk factors: resistance of the host and dose of external bacteria.
Healthy patients have a better chance of recovering from surgery without complications. According to National Institutes of Health (NIH), diabetes, cigarette smoking, obesity and existing comorbidities in patients add to the risk of SSI. Health care providers can help increase a patient’s resistance to bacteria by instructing them to follow protocols including eating a healthy diet, avoiding smoking and getting rest prior to their procedure. This is recommended but hard to enact.
The environment is where one has the greatest influence. The patient themselves and anything they come in contact with may introduce additional contaminants. That dose of bacteria, and other microbes, can be reduced through the proper use of sterilization of instruments and equipment, and surfaces in the room, administration of preoperative prophylactic antibiotics, and proper pre-operative preparation of patient’s skin and nares to reduce microbial load.
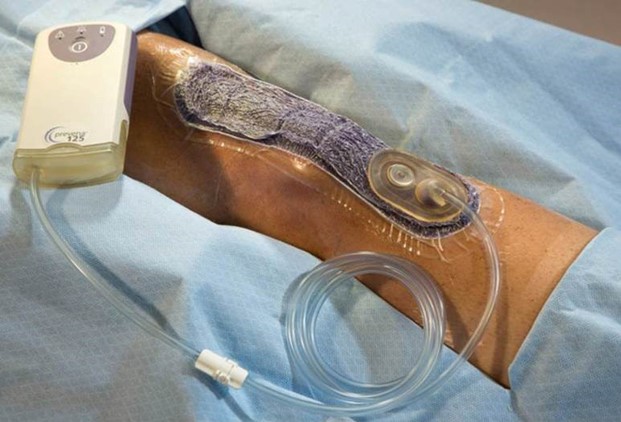
Another important part of reducing the risk of infection takes place at the end of the case with surgical incision management.
Surgical Incision management: What’s right for your patient?
Ways to increase resistance of the host
- Manage patient risk factors pre-surgery
- Temperature management
- Other (blood loss, glucose, deep vein thrombosis prevention)
Ways to decrease the dose of bacteria
- Sterilization and cleaning monitoring
- Prophylactic antibiotics
- Surgical preparation
- Prevention of environmental contamination
- Surgical incision management
With all the effort and care that goes into preparing for and completing the surgery, it’s important to continue that vigilance at the end of the case and in the following days and weeks post-surgery. Management of the incision site and choosing the best post-op dressings is key in reducing the risk of SSI.
Thankfully, the days of only having the option of a simple tape and gauze dressing over an incision have mostly passed. Today, a wide range of dressings and products are available – and you can choose the best dressing for your patient.
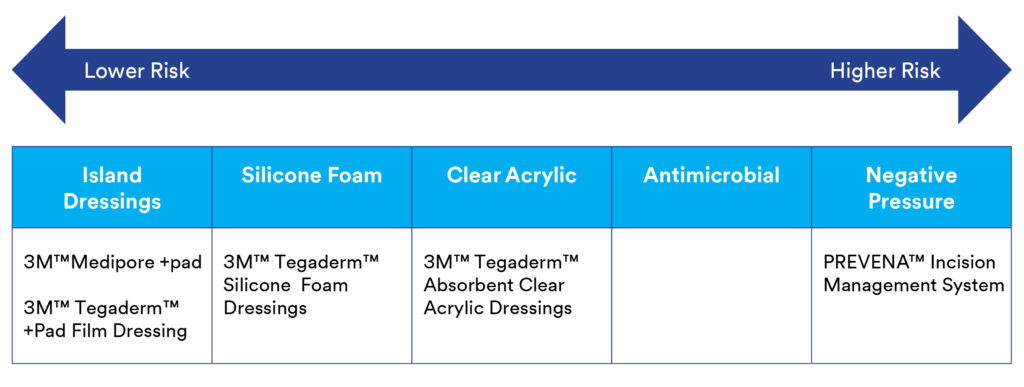
If a patient is assessed to be at lower risk for infection due to their underlying health, type of procedure, and surgical site status, and if a minimal amount of drainage of the incisional site is expected, some simple, yet effective, solutions are available. For medium- to high-risk situations, the dressings become more advanced and more high-tech. Additional solutions can better address high-risk patients, operations which may present with challenges of post-operative swelling, drainage, or skin health concerns.
For lower-risk cases
Basic island dressings – an absorbent sterile pad with a non-woven adhesive backing, or waterproof adhesive backing – can provide very good protection that meets the patient’s needs. Examples include:
- 3M™Medipore +Pad for an easy, all-in-one sterile and breathable dressing
- 3M™ Tegaderm™ +Pad Film Dressing for a waterproof1 barrier to keep the site isolated
For medium-risk cases
Silicone foam or clear acrylic dressings can provide protection and the ability to monitor the wound.
- 3M™ Tegaderm™ Silicone Foam Dressings that absorbs higher levels of drainage and provides gentle protection for fragile skin
- 3M™ Tegaderm™ Absorbent Clear Acrylic Dressings so caretakers can provide adequate absorption with the ability to monitor the surgical site without disturbing the incision.2,3
For higher-risk cases
Antimicrobial dressings or a negative-pressure system may be the best option.
- The PREVENA™ Incision Management System protects the incision from external contamination, helps hold incision edges together, removes fluid and infection materials, and delivers continuous negative pressure for up to seven days. Additionally, PREVENA Therapy is the first and only medical device indicated to aid in the reduction of superficial surgical site infections (SSIs) in patients at a high risk for post-operative infections in Class I and II wounds.
Surgical Closed Incision Management
Choose the best option for your patient
Preventing SSIs is a mission that we share across the healthcare industry. No single solution exists, but we can follow processes to manage variables before, during and after surgery. To provide the best incision management care, we can partner with you on education and training, and we can help you analyze and improve your practice.
Have questions?
References:
1 3M data on file. EM-05-014684
2 3M data on file. EM-05-000138
3 3M data on file. EM-05-000003
