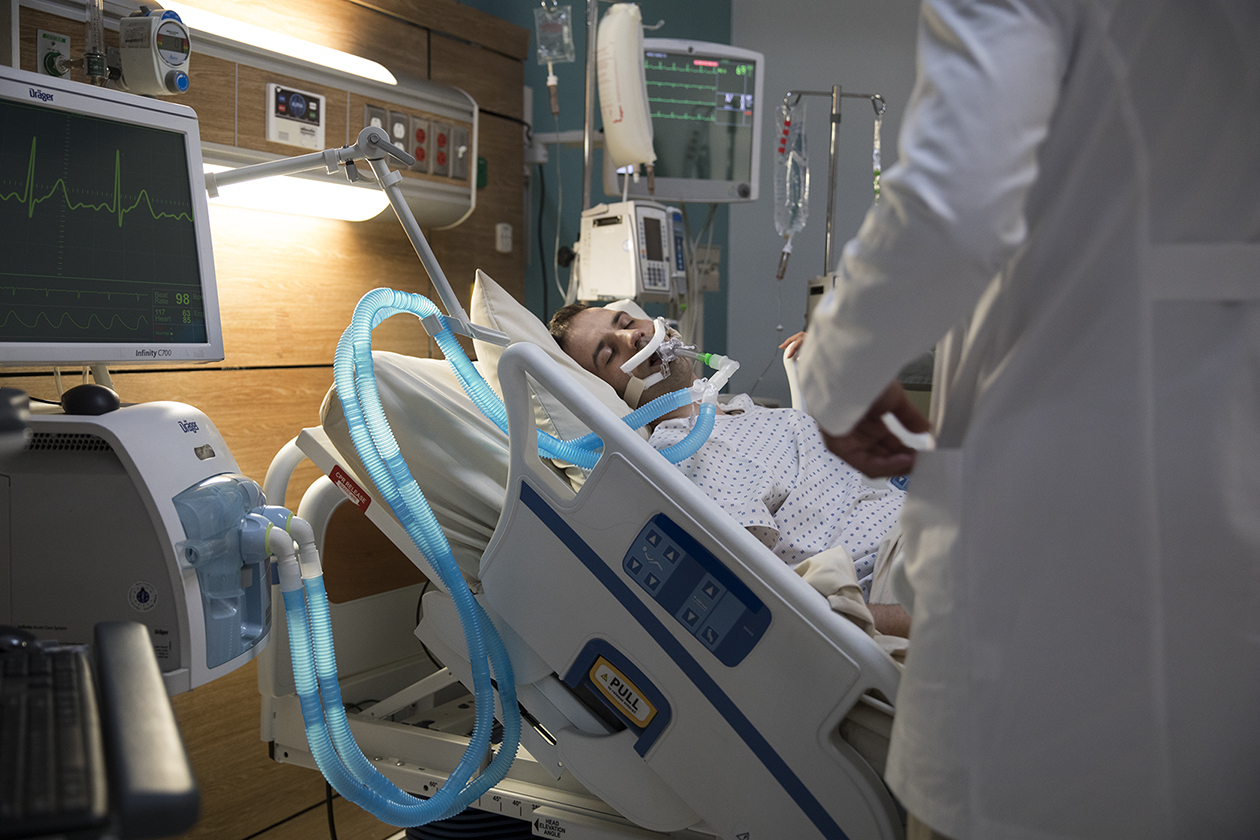
As clinicians, we understand that medical devices are critically important in the care of our patients. Almost every hospital patient will require at least one medical device for their care and treatment Unfortunately, medical equipment/devices that are used to save lives can also lead to pressure injuries. For instance, oxygen tubing or masks used to help improve patients’ oxygen saturation or orthopedic braces for fixation and/or mobility may cause a pressure injury. We also need to keep in mind the other devices our patients use every day-remote controls, cell phone chargers, eating utensils, and more-may cause pressure injuries. It is a good idea to keep your eyes open to all the ways medical and personal devices can put our patients at risk for a medical device or non-medical device-related pressure injury. It is our job as bedside clinicians to help prevent skin damage, such as pressure injuries.
Medical Device Related Pressure Injuries (MDRPI) are not new and account for about 30% of hospital-acquired pressure injuries. MDRPI increases the risk of potentially life-threatening infections, such as sepsis. They cause pain and can leave scars, which may be highly visible and cause distress. They may result in permanent hair loss, altered body image, and/or reduced quality of life. And last, they may increase the length of hospital stays and consume additional resources (time and products).1,2
Risk factors for developing an MDRPI include: being over 75 years old, having impaired mobility, impaired microclimate of the skin, compromised nutrition, and dependence on medical devices for survival.1,3
Common Devices that may cause injury include:
- Feeding tubes
- Oxygen delivery tubes
- Intravenous catheters
- Foley catheters
- Catheters
- Orthopedic devices
- Restraints
- Negative pressure wound therapy
- Bedpans
- Abdominal binders
- ID bands
- Braces
- Casts
In addition to Medical Devices, we must also consider other Device Related Pressure Injuries caused by:
- Remotes
- Pens
- Phones
- Glasses
- Hearing aids
- Food & personal items
These items may be lost in the bed and cause pressure on a patient who is unable to sense the object or who is immobile.1,3
Preventative Strategies:2
Assessment: A comprehensive skin assessment can help lead us to proper identification and early prevention. It is critical to assess the skin underneath a medical device to identify the early signs of pressure.
Positioning: Position and reposition the patient and the device to help redistribute pressure and decrease the shear force. Remove the device as soon as medically feasible.
Education: Educate staff and patients on preventive measures and pressure injury potential.
Device care: Ensure that the patient receives the proper size and type of device; that the device is secure, to decrease movement or slippage; that the skin is padded, to reduce friction; and that the manufacturer’s recommendations for use and care of the device are followed.
Documentation and communication: Ensure that the patient’s assessment, interventions, and continuing care needs are communicated and documented.
Teamwork: Work with all care team members to create and implement the patient’s care plan.
To learn more about pressure injuries, please view our pressure injury resources page. It has multiple articles, tools, and a series of 5-minute educational videos to help you and your team.
