 The numbers are in. In the US, outpatient clinic visits dropped by 60% during the initial response to the COVID-19 pandemic.1 Now, after several months, visits are starting to rebound as systems resume services, testing and procedures, but remain roughly one-third lower than pre-pandemic volumes. What does this mean for the VLU patient? We know that many wound clinics were forced to reduce their patient volumes or close completely during this time of crisis. Patients, most of whom are considered high risk, may have avoided seeking medical care due to fear of contracting the virus.
The numbers are in. In the US, outpatient clinic visits dropped by 60% during the initial response to the COVID-19 pandemic.1 Now, after several months, visits are starting to rebound as systems resume services, testing and procedures, but remain roughly one-third lower than pre-pandemic volumes. What does this mean for the VLU patient? We know that many wound clinics were forced to reduce their patient volumes or close completely during this time of crisis. Patients, most of whom are considered high risk, may have avoided seeking medical care due to fear of contracting the virus.
As a result, patients that had once been seen weekly for assessment, debridement and treatment were forced to be managed in alternative ways.
This included telehealth assessments, referrals to home care, triaging to alternate providers (such as primary care) or instructing the patient or family members to assume increased responsibility for wound management and monitoring. It’s not unusual for outpatient providers to have patients drop off the grid. There are various reasons – being ill, growing weary of the weekly visits or deciding the wound was “pretty close to healed”. But now, as the doors reopen, wound clinic staff are faced with the return of patients that may have had less than optimal care due to circumstances beyond their control. For a patient with VLUs, this is especially challenging.
Clinical Considerations
Restore skin integrity.
The dynamic of poorly controlled edema and increased wound drainage sets the stage for wet, irritated and vulnerable skin. This, combined with dressings that may not absorb adequate amounts of exudate or that are not changed at appropriate intervals, can lead to periwound maceration.
Plan: Protect periwound skin from the effect of maceration by using a moisture barrier film with each dressing change. Select a dressing that will manage high volumes of exudate such as a superabsorber or foam dressing. Finally, routine cleansing and moisturizing of the skin with each visit will keep the skin moisturized.
Manage the infection/biofilm.
Research has shown that 90% of chronic wounds have biofilm present.2 Biofilm creates a protracted inflammatory response that disrupts the wound healing process. In some cases, this can contribute to localized or spreading infection. Patients returning to clinics may have overt, easily recognized signs of infection including increased pain, odor, drainage, erythema and warmth. But the presence of biofilm may be less easy to discern – subtle signs can include friable tissue quality, repeated accumulation of fibrinous debris on the wound surface or simply a non-progressing or “stalled” wound.
Plan: Treat biofilm aggressively. Strategies include debridement and topical antimicrobial agents that are specifically effective against biofilm (Note: Some dressings identified as “antimicrobial” are effective only on planktonic bacteria and not bacteria protected within a biofilm). Wounds with signs of spreading infection may require systemic antibiotics. When the wound begins to progress, reassess the need for the ongoing use of antimicrobials.
Control edema.
Reduction or elimination of edema is the key principle of VLU management. Without therapeutic compression, healing may be delayed, wound exudate and leg discomfort (aching, fatigue) can increase. Immobility activity restrictions, brought on by COVID-19 precautions, combined with inadequate or a lack of compression can contribute to edema for patients with VLUs.
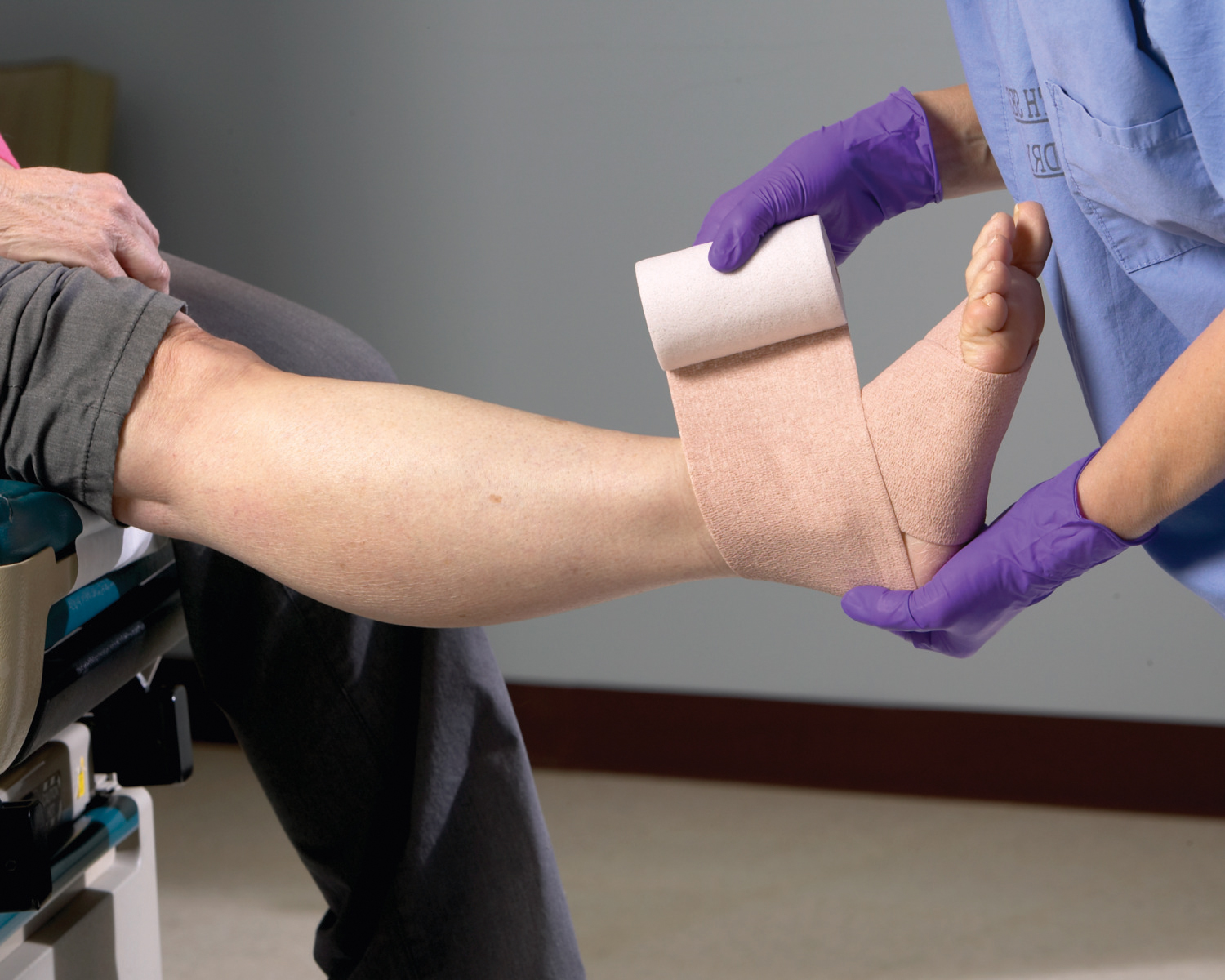
Plan: Upon verifying adequate perfusion, initiating (or resuming) compression is essential. Anticipate increase wound drainage volumes and decrease in leg circumference as fluid shifts from interstitial spaces back into the vascular system. Review the importance of exercise (ambulation or calf raises) and leg elevation in the comprehensive effort to combat edema.
Provide support to patients and their caregivers.
Most of us have never had to try to clean and dress a painful wound on our outer ankle then squeeze our swollen leg into a compression stocking. Most of us haven’t had to shop for the cheapest source of gauze dressings because our leg was dripping and we couldn’t see a medical provider. Managing a non-healing wound, combined with the psychosocial stress related to the pandemic (isolation, fear of illness, financial concerns) can contribute to anxiety, depression and associated conditions.
Plan: Determine the strategy for VLU management that is best for each individual patient. Your clinic may not be able to immediately return to “business as usual” and your patients may not be ready for that. The routine, weekly visit protocol for VLU patients may need to be adjusted. This could mean telehealth visits or collaboration with home care nursing. Many clinics are adding phone call check-ins as a way of staying in touch and identifying potential concerns for patients with less frequent clinic visits. Finally, some clinicians are finding that this time of uncertainty is inspiring patients and caregivers to take an increased ownership in wound treatment. In-person instruction as well as educational resources (digital and print) reinforce the prescribed plan of care.
VLUs are one of the most common types of wounds managed by outpatient wound clinics. However, there is nothing “common” about the challenges that clinics and their patients are currently facing. Now is the time to take the framework of best practice principles and modify it as needed to create a new (and perhaps improved) approach to VLU management.
As we adjust our approach, we also know little changes can make a big difference. Download this reference guide to share with your patients.
References:
Mehrotra, A., Chernew, M., Linetsky, D., Hatch, H., & Cutler, D. (May 19, 2020). The Impact of the COVID-19 Pandemic on Outpatient Visits: A Rebound Emerges. Retrieved from https://www.commonwealthfund.org/publications/2020/apr/impact-covid-19-outpatient-visits
Attinger, C., Wolcott, R. Clinically Addressing Biofilm in Chronic Wounds. Adv Wound Care. 2012;1(3):127-132.
