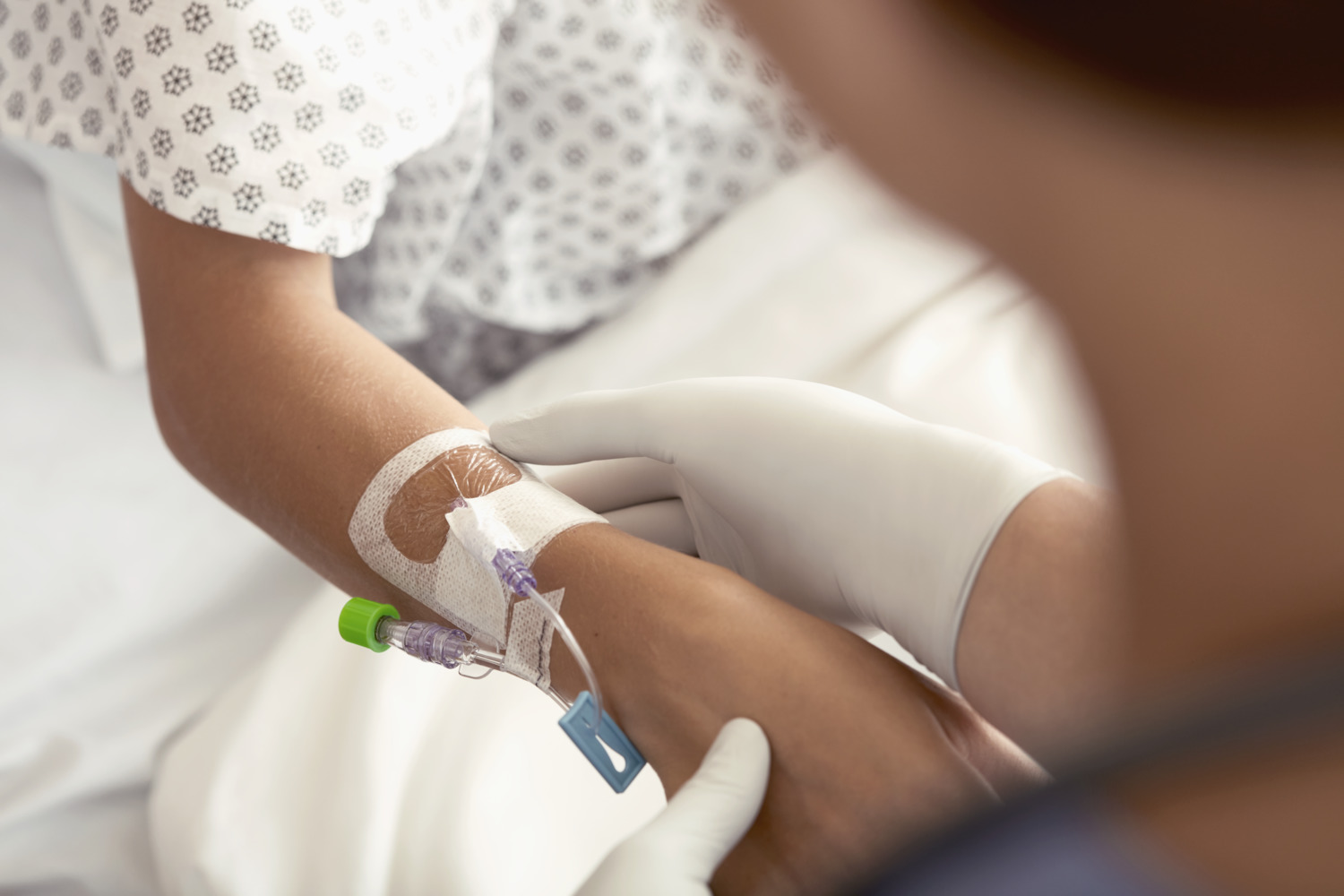
We all know science is crucial to medicine and obtaining the best outcomes. After all, evidence-based outcomes are the backbone of care. However, in some areas, that science merges with art – the two working in concert to deliver the best care.
January 25th is IV Nurse Day and we asked several 3M employees with experience in infusion therapy to talk about the day, the role of infusion therapy and how technology in the field has changed. Their answers spoke to how the science and art of infusion therapy are woven together.
What does IV Nurse Day mean to you?
 Kris Hunter, RN, BSN, CRNI, VA-BC: I see IV nurse day as a recognition of infusion therapy as a practice. It’s a critical clinical practice that spans almost all clinical settings and is often prominent in the most critical settings. The art of infusion therapy can mean something as simple as whether the patient has a good day or not or be as important as life or death.
Kris Hunter, RN, BSN, CRNI, VA-BC: I see IV nurse day as a recognition of infusion therapy as a practice. It’s a critical clinical practice that spans almost all clinical settings and is often prominent in the most critical settings. The art of infusion therapy can mean something as simple as whether the patient has a good day or not or be as important as life or death.
What led you to pursue certifications in infusion therapy?
Kris: I chose certification for the structured learning. I wanted to be the best infusion therapy nurse that I could be; that is what my patients deserved. Nursing is an art that requires continuous practice and learning not just to become great but merely to maintain basic proficiency.
What sparked your initial interest in infusion therapy?
 Robin Huneke Rosenberg, MA, RN-BC, CRNI, VA-BC: When I began working at Children’s Minnesota in 1989, I was afraid to start IVs. However, working in the Emergency Room I quickly had to learn. I soon realized that starting IVs is not only a skill, but also a therapy where education and understanding is required for the patient and family. I then began providing outreach courses in pediatric I.V. therapy throughout the Twin Cities and Minnesota. Eventually, I pursued my graduate degree in nursing education as I developed and implemented Children’s first vascular access program in 2007, transforming how I.V. access and I.V. therapy was delivered for the hospitalized child.
Robin Huneke Rosenberg, MA, RN-BC, CRNI, VA-BC: When I began working at Children’s Minnesota in 1989, I was afraid to start IVs. However, working in the Emergency Room I quickly had to learn. I soon realized that starting IVs is not only a skill, but also a therapy where education and understanding is required for the patient and family. I then began providing outreach courses in pediatric I.V. therapy throughout the Twin Cities and Minnesota. Eventually, I pursued my graduate degree in nursing education as I developed and implemented Children’s first vascular access program in 2007, transforming how I.V. access and I.V. therapy was delivered for the hospitalized child.
Kris: Infusion therapy chose me. By chance I was thrown into an infusion therapy position and grew to love the art. I liked the detailed technical aspects of gaining vascular access and delivering various therapies. There is something extremely satisfying about counting the drops of a liter bag of fluids and getting the timing correct down to the minute.
 Kim Schommer, RN, BSN, VA-BC: While working in the hospital, inserting IVs and managing them was a daily task that was just part of the job. I knew it had an important impact on patient care, but it wasn’t until my role at 3M that I truly understood the value. It’s now become important to me to educate others on providing the correct care because of the impact I know it has on patient outcomes.
Kim Schommer, RN, BSN, VA-BC: While working in the hospital, inserting IVs and managing them was a daily task that was just part of the job. I knew it had an important impact on patient care, but it wasn’t until my role at 3M that I truly understood the value. It’s now become important to me to educate others on providing the correct care because of the impact I know it has on patient outcomes.
With so many disciplines potentially working with vascular access, how does the role of infusion nurse specialist affect patient care?
Robin: The role of an infusion nurse is dedicated to safe patient care: providing I.V. therapy to the right patient, identifying the correct administration method and location for prescribed medications, to infuse medications over the right amount time and observing patient for signs and symptoms of complications. Infusion nursing is not just about vascular access – it also includes intrathecal (intraspinal), subcutaneous delivery methods and practices in addition to maintenance and site cares for the vascular access site based on evidence-based practices.
What changes in the world of infusion therapy have been most interesting to you? What have been the biggest changes?
Kris: Infusion therapy has been at the center of aggressive cost control efforts in the scientific research arena and federally. The Pay-for-Performance program with the CLABSI initiative is a good example of the government driving an improvement in healthcare while controlling costs.
Kim: Understanding the role vascular access and blood stream infections play in patient care. The attention that is placed on the care of lines, the technology we now have that ensures insertion can be done appropriately the first time and tools to avoid sticking a patient multiple times for blood samples all help improve the patient experience.
